Saving Lives One Call at a Time
By Michael Cunningham
Heinz College students and faculty develop a technology solution to help ER doctors get the information they need to make critical decisions as patients arrive at the ER.
If you’ve ever watched “ER” or “Chicago Med,” you’ve probably witnessed a chaotic portrayal of the emergency room intake process. Nurses and EMTs scream at each other, practically sprinting to wheel a critical patient into surgery. A surgeon analyzes a clipboard that somebody just shoved into her face, using her free hand to attempt to stop a patient from bleeding. All the while, precious seconds are ticking away that could mean the difference between life and death.
For Dr. Shiv Dua (MSHCPM ’09), a resident physician in emergency medicine at Allegheny General Hospital and Heinz College alumnus, television’s portrayal of the ER is not merely fictional or dramatized. It is his daily reality.
“I’m trying to stabilize an acutely ill patient, and then there’s multiple conversations,” he said. “There’s an ER nurse talking to a flight nurse. I can’t listen to that conversation because I’m trying to figure out what’s going on with this patient.”
And that’s just on the intake end of the ER. Critical patients are transported to hospitals in a variety of ways – by ambulances, private vehicles, and aeromedical helicopters. While a patient is being transported to a hospital, first responders such as paramedics, flight nurses, and EMTs are administering treatments to the patient in transit and having conversations with the hospital’s receiving care team about what they are observing and what actions they are taking.
All of these conversations and first-response treatments generate critical information that receiving ER physicians should have in a digestible format, so that they can utilize it to make potentially life saving decisions at the point of care.
But in many cases, the receiving ER physicians don’t gain access to this information at all, because they aren’t on the receiving care team that was in contact with the first responders. And when they do receive this information, it is in the form of clunky conversation transcripts or 300-page printouts of medical records.
“A lot of what we deal with is trying to make sense of what we’re seeing in a very quick amount of time with very limited information,” said Dr. Dua. “A lot of the information that we do get is not relevant. The relevant pieces that I wish I had, I don’t have. There are some things we repeat. There are things we didn’t know when the patient got into the hospital that would have never been captured, and we don’t have an elegant way of capturing them.”
To develop a solution to this problem that he described as “systemic,” Dr. Dua and his colleague, Dr. Paul Porter, reached out to Rema Padman, Heinz College Professor of Management Science & Healthcare Informatics, and a team of current Heinz College students.
The interdisciplinary team, consisting of students from the Master of Health Care Policy and Management (MSHCPM), Master of Information Systems Management (MISM) and Master of Public Policy and Management (MSPPM) programs, spent the fall semester developing a proof of concept technology solution for Allegheny General Hospital for their capstone project.
[This app] can absolutely save lives. It advocates for patients in their highest time of need.Dr. Shiv Dua
"We know they are capturing some of this data, including phone conversations between paramedics and hospital-based physicians,” said Padman. “But these are all voice files. So how do we convert these voice files into text files, and then how do we extract relevant data from the text files to briefly summarize critical information that the receiving care team can quickly browse through?”
To achieve this goal, the students used an application program interface (API) to convert all the audio conversations to a text format, where they then categorized the conversations based on keywords into diagnoses, symptoms, and medications.
“We used Google API to transcribe and convert the audio to text,” said Torrell Jackson, the project manager and a joint MSCHPM-MBA student. “Then we used another tool to extract key terms from the text and categorize everything. So we were able to really marry two already existing technologies and consolidate the information to benefit the hospitals in the long run.
“We brought all these elements together so that information was presented in a way in which the physicians would be able to receive it and look over it before the patient arrived.”
The app combines the talk-to-text information and the patient’s medical records into a one-page PDF document that ER physicians can quickly peruse to get all of the relevant information they need at the point of care. And Jackson hopes that future Heinz College students will continue this research so that the output can actually be integrated into the patient’s medical records.
“Ideally, when they continue this project next year, they’re going to convert it and implement it within a person’s electronic health record,” Jackson said. “So before the patient even comes, as long as they’re registered in the system, the ER physicians will be able to have this document with this conversation implemented directly into the patient records. Therefore, no matter who touches the patient and when, they have at least an idea of what the patient experiences were prior to getting to the hospital.”
“There are great opportunities to leverage this initial solution to develop such extensions through additional capstone projects as well as via rigorous research studies that will provide a strong foundation for the technology artifacts,” suggested Padman.
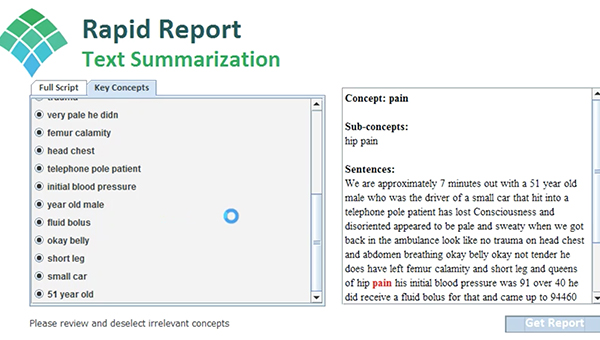
RAPID REPORT
Here's a peek at the interface of AGH Rapid Report, a demo of which was presented to the client.
Dr. Dua said he was “blown away” by the proof of concept implementation, and said that he is looking forward to further collaborating with Heinz College students to build out this application.
“I think it can absolutely save lives,” he said. “I think it advocates for patients in their highest time of need, and in their most nerve-racking time. The emergency room is a scary place for a patient. You forget details. You may not even be able to talk if you’re that sick, and you’re relying on other people to collect the information for you. And as a physician, if you can collect this information from different data streams and make it useful, that is incredibly important.”
And for Jackson, who has lost family members to cancer at a young age, participating in the project simply reaffirmed why he decided to study health care at Carnegie Mellon University.”
“When you really think about it, every person means the world to somebody else,” Jackson said. “Being able to impact one person’s life, you understand that, in helping to save one person’s life, you’re actually impacting their entire family. So this project is amazing, because you ultimately have the opportunity to impact thousands of lives in a positive way, which is why I was interested in health care in the first place.”
“This capstone project is truly illustrative of our ability to address some complex and challenging problems in the healthcare domain by bringing together the unique, interdisciplinary strengths of our students from multiple programs with the critical, real-world needs of acutely ill patients and time-constrained clinicians,” concluded Padman.
Learn more about the MSHCPM Program